Foundations in Microbiology
10th Edition
ISBN: 9781259705212
Author: Kathleen Park Talaro, Barry Chess Instructor
Publisher: McGraw-Hill Education
expand_more
expand_more
format_list_bulleted
Textbook Question
Chapter 20.L2, Problem 1VC
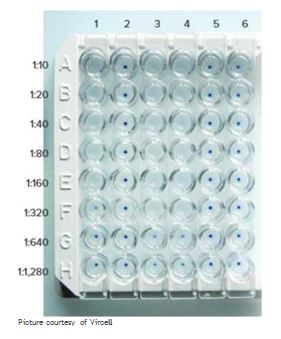
Use figure 20.5 a, b as a reference guideline for interpretation. Lanes numbered 1 through 6 are different patient sera and A through H are increasing dilutions of these sera. Identify the samples that show Brucella infection and give their titers. Which positive sample has the fewest antibodies? What conclusion can be made if a second test done on this same patient a week later indicates no change? What is the conclusion if all lane wells are positive for this patient?
Expert Solution & Answer
Want to see the full answer?
Check out a sample textbook solution
Students have asked these similar questions
An ELISA was performed on the sera of three patients to detect antibody against varicella
(the chickenpox). Give the titer results shown in the answers, which patient's serum had the
most anti-varicella antibody?
There is not enough information to answer the question.
Patient 2, dilution 1:30
O Patient 1, dilution 1:2,000
O Patient 2, dilution 1:400
When a patient exhibits a four-fold or greater rise in antibody titer against a specific microbial antigen between acute-phase and convalescent-phase serum samples, this is considered to be a “seroconversion”. Which of the following would be a correct interpretation of a seroconversion?
what option below is the answer?
None of the other four answers are a correct interpretation of a seroconversion
These results show that the microbe itself has been detected in the patient’s sample(s)
These findings cannot be interpreted because antibodies aren’t specific enough for antigens
There is no evidence of current active infection because that would require that the antibody titer is decreasing rather than increasing
The results show evidence of current or recent infection by the specific microbe because there has been an active immunologic response to its antigen
At time point A, the patient's IgG titer against antigen X is 1:6, the patient's IgM titer to the same antigen is zero. Later, at time point B, the same patient again encounters antigen X. The IgG titer is zero, and the IgM titer to X is 1:8. Describe a scenario that could explain these data.
Chapter 20 Solutions
Foundations in Microbiology
Ch. 20.1 - Explain the effect of the virulence factor common...Ch. 20.1 - Identify those people most at risk of developing a...Ch. 20.1 - Briefly describe the human infections caused by...Ch. 20.1 - How can antibiotic treatment of a gram-negative...Ch. 20.2 - Name the genera of bacteria that are...Ch. 20.2 - Outline the pathology and epidemiology of...Ch. 20.2 - Explain the epidemiology of Francisella tularensis...Ch. 20.2 - Prob. 6ELOCh. 20.2 - Prob. 7ELOCh. 20.2 - Prob. 8ELO
Ch. 20.2 - List the four genera of bacteria that cause...Ch. 20.2 - Prob. 4CYPCh. 20.2 - Prob. 5CYPCh. 20.2 - Prob. 6CYPCh. 20.2 - What is unusual about the reservoir of Legionella?...Ch. 20.3 - Recall the medically important members of the...Ch. 20.3 - Prob. 10ELOCh. 20.3 - Explain the importance of the three major surface...Ch. 20.3 - Name the key characteristics shared by the...Ch. 20.3 - Explain what is meant by IMViC.Ch. 20.3 - Prob. 10CYPCh. 20.3 - Prob. 11CYPCh. 20.3 - Briefly describe the methods used to isolate and...Ch. 20.3 - Prob. 13CYPCh. 20.4 - Differentiate among the major enteric pathologies...Ch. 20.4 - Explain the role of E. coli in infantile and...Ch. 20.4 - Prob. 14ELOCh. 20.4 - Prob. 15ELOCh. 20.4 - Prob. 14CYPCh. 20.4 - Prob. 15CYPCh. 20.4 - Justify treating E. coli Ol57:H7 differently from...Ch. 20.4 - Prob. 17CYPCh. 20.4 - Prob. 18CYPCh. 20.5 - Differentiate between true noncoliform enteric...Ch. 20.5 - Distinguish the pathologies of typhoidal and...Ch. 20.5 - Identify the possible sources of Shigella...Ch. 20.5 - Prob. 19ELOCh. 20.5 - Prob. 20ELOCh. 20.5 - Prob. 19CYPCh. 20.5 - Prob. 20CYPCh. 20.5 - Make a comparison chart for Shigella and...Ch. 20.5 - What are the Five F’s and how do they relate to...Ch. 20.5 - Prob. 23CYPCh. 20.5 - Which body systems are commonly infected by...Ch. 20.5 - Describe the epidemiology and pathology of...Ch. 20.L1 - A unique characteristic of many isolates of...Ch. 20.L1 - Prob. 2MCQCh. 20.L1 - Prob. 3MCQCh. 20.L1 - A classic symptom of pertussis is a. labored...Ch. 20.L1 - Prob. 5MCQCh. 20.L1 - Prob. 6MCQCh. 20.L1 - Prob. 7MCQCh. 20.L1 - Which of the following is a major difference...Ch. 20.L1 - A complication/complications of typhoid fever...Ch. 20.L1 - Prob. 10MCQCh. 20.L1 - Prob. 11MCQCh. 20.L1 - Haemophilus influnzae is ____________ and requires...Ch. 20.L1 - Prob. 13MCQCh. 20.L1 - Prob. 14MCQCh. 20.L1 - Single Matching. Match the infectious agent with...Ch. 20.L1 - Prob. 1CSRCh. 20.L1 - Prob. 2CSRCh. 20.L1 - Prob. 3CSRCh. 20.L1 - Prob. 1WCCh. 20.L1 - What are unique features in the epidemiology of E....Ch. 20.L1 - Explain several practices an individual can use to...Ch. 20.L1 - Prob. 4WCCh. 20.L1 - Briefly outline the zoonotic infections in this...Ch. 20.L2 - What is the logic behind testing for E. coli to...Ch. 20.L2 - Identify the genera with the following...Ch. 20.L2 - Given that so many infections arc caused by...Ch. 20.L2 - Prob. 4CTCh. 20.L2 - Students in our classes sometimes ask how it is...Ch. 20.L2 - Explain lhe reasons for an increase in numbers of...Ch. 20.L2 - Compare and contrast the pathology, diagnosis, and...Ch. 20.L2 - Prob. 8CTCh. 20.L2 - Prob. 9CTCh. 20.L2 - Prob. 10CTCh. 20.L2 - "There is no circumstance [in which] you can cook...Ch. 20.L2 - Use figure 20.5 a, b as a reference guideline for...
Knowledge Booster
Learn more about
Need a deep-dive on the concept behind this application? Look no further. Learn more about this topic, biology and related others by exploring similar questions and additional content below.Similar questions
- When a patient exhibits a four-fold or greater rise in antibody titer against a specific microbial antigen between acute-phase and convalescent-phase serum samples, this is considered to be a "seroconversion". Which of the following would be a correct interpretation of a seroconversion? None of the other four answers are a correct interpretation of a seroconversion These findings cannot be interpreted because antibodies aren't specific enough for antigens There is no evidence of current active infection because that would require that the antibody titer is decreasing rather than increasing These results show that the microbe itself has been detected in the patient's sample(s) The results show evidence of current or recent infection by the specific microbe because there has been an active immunologic response to its antigenarrow_forwardDepending on the purpose, the typhoid fever can be diagnosed in the laboratory by either of the following method, i) Widal, ii. Blood culture and iii. Nucleic acid based identification method. Write a brief essay comparing these three diagnostic tests. Your answer must contain the basis of identification of each test, what does it mean by positive and negative results and which test do you think to be useful for the identification of active patient and which test is/are useful for the screening of previously infected case. Which test is prerequisite to perform the antibiotic susceptibility pattern?arrow_forwardA technologist failed to notice that the centrifuge had not properly centrifuged the test tubes prepared for antibody identification. The time of centrifugation was 15 seconds instead of 30 seconds. What would be the potential error in the interpretation of this test? can please any one provide me ans?arrow_forward
- Why monoclonal antibodies method is better than polyclonal antibodies method in detecting specific pathogen? Explain the reasons for both selection or rejection methods..arrow_forwardYou just received the properly labeled blood bank specimen on patient Aran Stark. You decide to collect some background information about her known historical antibodies before beginning the work-up knowing that she has a history of anti-E, anti-K, anti-Jk^a, anti-Fy^a, anti-M and anti-Le^a. When you complete the work-up, you note that the anti-Jk^a antibody is no longer detectable. Can the patient receive red blood cells that contain the Jk^a antigen? Why or why not?arrow_forwardRea performed a quality control on hematology section. She noticed that results were out of range for the normal control. The tests were repeated twice and produced same result. What must be the most probable reason for this scenario? How should she address this problem?arrow_forward
- You just received the properly labeled blood bank specimen on patient Aran Stark. You decide to collect some background information about her known historical antibodies before beginning the work-up knowing that she has a history of anti-E, anti-K, anti-Jk^a, anti-Fy^a, anti-M and anti-Le^a. Which antibody can be neutralized? Which antibody is destroyed with 0.2M DTT treatment? Which antibody reactivity is enhanced by acidification? Which of the antibodies that are typically IgG in nature are destroyed by enzymes? Which are enhanced by enzymes? Which of these antibodies have been known to cause hemolytic transfusion reaction? Which of these antibodies are known to react at room temperature? Which of these antibodies react best at 37C? * When you complete the work-up, you note that the anti-Jk^a antibody is no longer detectable. Can the patient receive red blood cells that contain the Jk^a antigen? Why or why not?arrow_forwardA 38 year-old woman went to a hospital and complained of a non-productive cough and dyspnea which has progressed over two weeks. Based on physical examination, she was pale, diaphoretic and in acute respiratory distress. According to her, she had a sexual contact with his partner for the past weeks. The physician ordered laboratory tests and results revealed that the CD4 count was significantly low. Questions:What might be the predominant antibody present in the patient’s serum and why? What immunological response the patient’s body will develop and why?arrow_forwardWhy monoclonal antibodies method is better than Polyclonal Antibodies method in detecting specific pathogen. Explain reasons.arrow_forward
- Why test that mice infected with B. anthracis produce antibodies to the S-layer proteins? What is the point, what does it tell us? (figure 6) I need help finding the answer in the article and answer as short a possible link to article: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC106848/arrow_forwardOf the 220 HIV-infected outpatients of the dermatological and venereological dispensary examined in 12, a positive result was obtained. The study was performed by solid-phase ELISA on polystyrene tablets to detect antibodies to HIV. Stage II serological diagnosis was applied to those who tested positive for ELISA to definitively establish the fact of HIV infection. There were 8 such persons. What is the principle of the method used in the first stage of serological diagnosis? Antibodies to which components of HIV are determined in ELISA? What is the diagnostic value of ELISA? What components are needed for the implementation of solid-phase ELISA? Which method should be used in the second stage of HIV detection to avoid overdiagnosis? What is the principle of immunoblotting? Antibodies to which components of HIV are determined by immunoblotting? According to the results of which serological method is the final diagnosis of HIV infection made?arrow_forwardIn a screening test for Chlamydia, the sensitivity is 83% and specificity is 50%. A total of 800 subjects were screened, of whom 90 actually had Chlamydia (confirmed through follow-up testing). Calculate and interpret the Positive and Negative predictive values.arrow_forward
arrow_back_ios
SEE MORE QUESTIONS
arrow_forward_ios
Recommended textbooks for you

Serology 101: Testing for IgG and IgM antibodies; Author: Beckman Coulter Dx;https://www.youtube.com/watch?v=LtqKB-qpJrs;License: Standard youtube license