
Concept explainers
Since the 1950s, when living kidney donation was first recognized as a viable alternative to cadaver organ donors, family and friends have come forward to offer a kidney to a victim of kidney failure. To reduce the chance that the recipient’s immune system will attack the donated kidney as if it were an invading microbe or
To remove a donor kidney (FIG. 36-9), surgeons generally use a technique called laparoscopic surgery, where they make half-inch incisions through which they insert surgical tools, including a tiny video camera to guide the operation. The kidney is extracted through an incision about 2½ inches long, put on ice, and rushed to its recipient. The operation takes 3 to 4 hours; donors remain in the hospital for about 3 days and return to work in about 3 weeks. In addition to the risks associated with major surgery, kidney donors will lack a backup kidney in the unlikely event that their remaining kidney fails. But a recent study of deaths among 80,000 kidney donors during a 15-year period found no greater mortality among this group (once they had recovered from their surgery) than among non-donors.
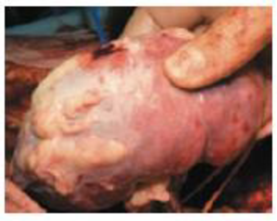
FIGURE 36-9 Surgeons transplant a kidney
Domino donations are almost always started spontaneously by someone inspired to make a difference. Since 2008, when DeGiulio’s donated kidney started a chain that saved four lives (FIG. 36-10), such domino donation chains have become longer and more frequent. For example, during a 4-month period, 17 hospitals in 11 states from California to New Jersey matched 30 people—who might otherwise have died—with kidneys from 30 donors they had never met. This heroic enterprise was started by Good Samaritan Rick Ruzzamenti, who got the idea from the desk clerk at his yoga studio, who had mentioned to him that she had donated a kidney to a friend. “People think it’s so odd that I’m donating a kidney,” he told the transplant coordinator at his hospital, but “I think it’s so odd that they think it’s so odd. . . . It causes a shift in the world.”

FIGURE 36-10 Domino donations Kidneys from compatible strangers saved the lives of these four recipients.
The more than 100,000 eligible individuals awaiting a kidney transplant ardently hope that domino donation chains continue to be forged and to lengthen.
CONSIDER THIS Would you donate a kidney to a friend or family member whose kidneys were failing? Would you consider donating a kidney to a stranger? Explain your reasoning.
Want to see the full answer?
Check out a sample textbook solution
Chapter 36 Solutions
Biology
- What is an agglutination response? How can it be avoided when blood is transfused?arrow_forwardWhy does the "rule of three" not applicable to non-normocytic and non-normochromic red blood cells?arrow_forwardMs. Wu, whose blood type is O-, requires a blood transfusion.Her family members volunteer to donate blood. Their blood types are as follows: her son, type B-; her husband, type B+; her daughter, type O+. Which family members could safely donate blood to Ms. Wu? Who could not? Explain.arrow_forward
- An individual demonstrates antibodies (A) and antibodies (B) in their blood. Their blood type would be which of the following? (A) AB+ (B) AB- (C) AB ? (presence/absence of Rh factor undetermined) (D) O+ (E) O- (F) O ? (presence/absence of Rh factor undetermined)arrow_forwardMs. House, a 32-year-old Hispanic woman, has had a history of intermittent pleuritic chest pain and joint pain for the past several years. Recently, she went to her physician because she noticed that an erythematous, butterfly-shaped rash had appeared on her face. Further lab tests indicated protein in her urine. Her blood test indicated the presence of numerous antinuclear antibodies, especially anti-DNA, and mature neutrophils containing nuclear material. A diagnosis of systemic lupus erythematosus (SLE) was made. Discussion Questions Discuss possible reasons why SLE was not diagnosed earlier. (See SLE—Clinical Signs and Symptoms.) Discuss how the presence of antibodies can cause such widespread damage in organ systems. (See SLE—Pathophysiology.) Discuss treatments for SLE and a prognosis for the patient in this case. (See SLE—Treatment.)arrow_forwardMs. House, a 32-year-old Hispanic woman, has had a history of intermittent pleuritic chest pain and joint pain for the past several years. Recently, she went to her physician because she noticed that an erythematous, butterfly-shaped rash had appeared on her face. Further lab tests indicated protein in her urine. Her blood test indicated the presence of numerous antinuclear antibodies, especially anti-DNA, and mature neutrophils containing nuclear material. A diagnosis of systemic lupus erythematosus (SLE) was made. Discussion Questions Discuss how the presence of antibodies can cause such widespread damage in organ systems. (See SLE—Pathophysiology.) Discuss treatments for SLE and a prognosis for the patient in this case. (See SLE—Treatment.)arrow_forward
- 66) A 68-year old man has a 1-month history of hemoptysis and weakness. He has smoked 2 packs of cigarettes per day for 50 years. Eyelid ptosis is present bilaterally. Muscle testing shows increasing strength during several seconds of effort. An X-ray of the chest shows a mass on the left upper lobe of the lungs . Antibodies are most likely to cross-react between the mass and which of the following? (A) Muscle mitochondria (B) Myofilaments (C) Na+ - K+ pump (D) Synaptic Ca2+ channels (E) Thyroid-stimulating hormone receptorsarrow_forwardA patient requires a blood transfusion after experiencing blood loss due to a traumatic injury. The patient's record lists their blood type as B+, Out of the following available options in the blood bank, what is the best type of donor blood to give to this patient? O Type A blood with antibodies removed via centrifugation O Type O- blood with antibodies removed via centrifugation Type AB+ blood with antibodies removed via centrifugation O Type O- whole bloodarrow_forwardA patient's antibody screen is resulted as positive. What should be done to test units for transfusion? Question 7 options: A) Antigen type the patient's red cells and crossmatch units positive for the same antigens. B) Determine the reacting antibody and crossmatch units negative for the corresponding antigen. C) Crossmatch ABO compatible blood at the immediate spin phase. D) Determine the reacting antibody and confirm that the donor did not have any similar antibodies.arrow_forward
- B" is a biomarker. Patients with higher concentration of "B" in their plasma have poor prognosis. Those patients are also resistant to a specific drug. So, alternative drugs are usually used to treat them. What kind of biomarker is "B"? Briefly explain.arrow_forwardApart from suffering from recurrent and prolonged infections, Denis Robin also experienced the following signs and symptoms: fatigue, rapid heart rate, pale skin, easy bruising, prolonged bleeding from cuts, and dizziness. Bone marrow transplant was not an option at that time and so blood transfusion was the treatment of choice. Explain the reasoning behind these other signs and symptoms that Robin experienced. Assume her blood group was A negative. Which blood groups can she receive? Which blood groups can she not receive? Explain why.arrow_forwardNeutrophils are best described as: (a) Phagocytic, have bilobed nucleus and are small (2-5 microns) (b) Respond to chemokines and are primary defense against bacteria (c) Long-lived phagocytic cells. why?arrow_forward
 Human Biology (MindTap Course List)BiologyISBN:9781305112100Author:Cecie Starr, Beverly McMillanPublisher:Cengage Learning
Human Biology (MindTap Course List)BiologyISBN:9781305112100Author:Cecie Starr, Beverly McMillanPublisher:Cengage Learning
